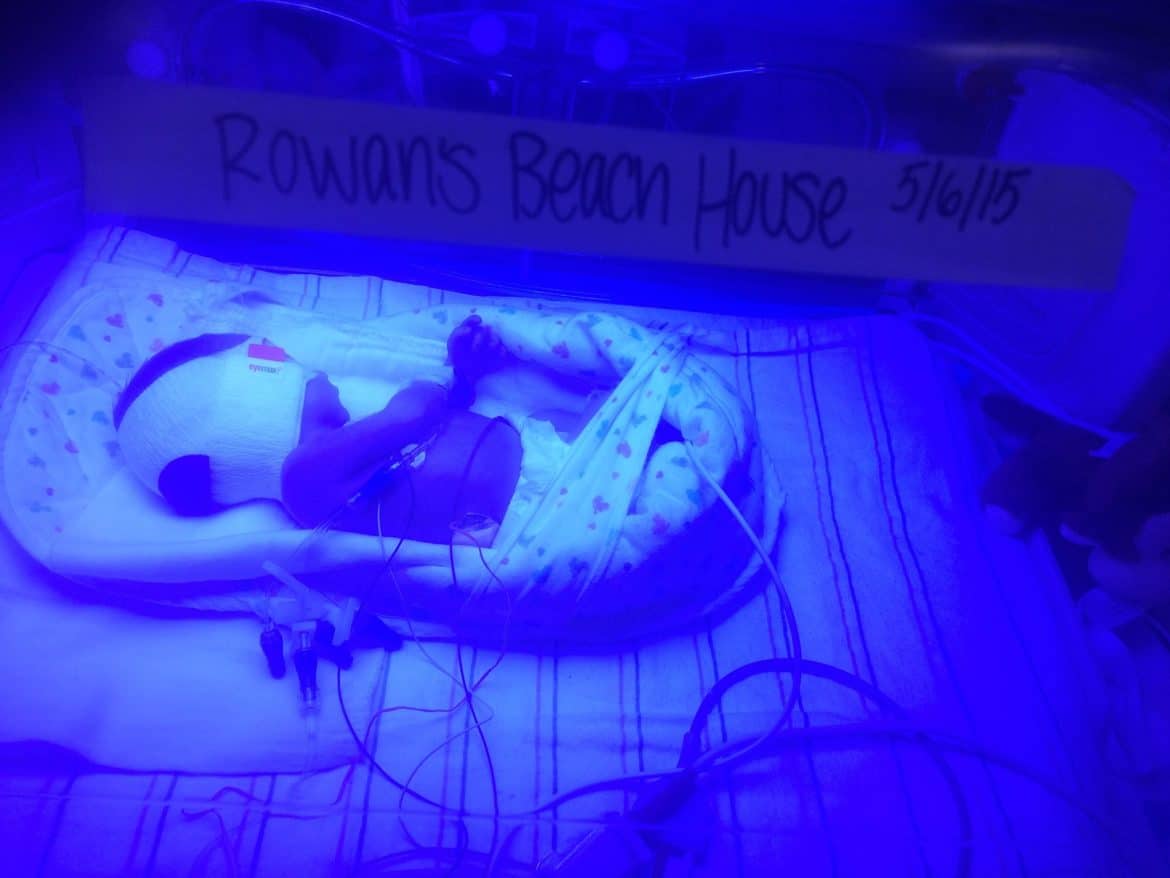
Even though around 60% of babies will experience some level of jaundice in their first week or two of life, it doesn’t make it any less scary for new parents.
What is jaundice
- Jaundice (hyperbilirubinemia) is the buildup of a pigment, called bilirubin, in your baby’s bloodstream. Bilirubin is a normal byproduct of the body breaking down old blood cells and is disposed of by our liver in bowel movements.
- During pregnancy, your liver takes care of it for both of you. After birth, however, it takes the baby’s liver a while to come online which allows bilirubin levels to increase (When in doubt, blame the liver).
- Approximately 60% of babies will experience some level of jaundice in their first week or two of life.
- This common type of jaundice, called Physiologic Jaundice, will generally appear within the first few days of life and disappear on its own within a couple of weeks (the timeline shifts later for premature babies).
Symptoms
- The rising levels of pigment creates a yellow cast to the skin and eyes. Essentially, your baby will begin to resemble a screaming Oompa Loompa.
- If you aren’t quite sure, press your thumb gently on baby’s forehead and then remove it. If the skin remains yellow, rather than blanching for a moment, it is likely there is mild jaundice at play.
- The level of jaundice can be *roughly* estimated by how far down the body the yellowish tone goes. A yellow face is less severe than when it progresses to the abdomen or feet.
- Baby can be difficult to waken, inconsolable when awake, and spend time arching her back. This is indicative of a more urgent situation.

Which babies are most at risk?
- Premature babies
- Babies who experience significant bruising during the birth, as they will have to break down more red blood cells.
- Mother/baby RH incompatibility
- Jaundice occurs at a higher rate in breastfed babies. Breastfeeding itself does not cause jaundice (except in rare cases of what is called “breastmilk jaundice”) but issues with intake can exacerbate it.
- In some cases there may be other disorders or issues at play, but these are rare.
Diagnosis
- Healthcare providers will check for jaundice during their normal rounds in the hospital.
- Many women, especially those who had a vaginal birth, will be out of the hospital before any noticeable symptoms arise, so your pediatrician will also be on the lookout during the appointment you schedule for your baby’s first week.
- In addition to the visual exam, your pediatrician may check bilirubin levels with a nifty light called a transcutaneous bilirubinometer (try to say that three times fast – or even once, at regular speed). It is pressed against baby’s toes, making her resemble a tiny E.T, while it gives a reading based on the reflection of light passing through the skin.
- Depending on the results of that screening and your provider’s assessment, a small blood sample may be taken for testing.

Treatment
- The potential for jaundice is one of several reasons you are sent home from the hospital with a fascinating chart to keep up with your baby’s urine output and bowel movements. Simply put, the more your baby eats, the more she poops. The more she poops the faster the bilirubin is flushed out of her system. Mild jaundice will frequently resolve on its own, without treatment, but should be monitored closely.
- Breastfeeding is a risk factor, a preventative measure, and a cure; the AAP recommends feeding your baby 8-12 times per day, for the first several days. This is also a great way to help your milk come in, which will further flush the bilirubin from her system. It’s the perfect time to schedule an appointment with a lactation consultant!
- Formula fed babies should have 1-2 ounces every 2-3 hours for the first week.
- Bili-lights – Your baby will be given some cool shades and turned into a tiny smurf while chilling under the blue lights. This light helps convert the bilirubin into a form more easily removed.
- Bili-blanket – Similar to the overhead lights, this is a fiber-optic blanket that your baby can hang out on to help flush the bilirubin. In some cases you can take one home with you, so you do not have to stay at the hospital just for jaundice therapy.
- For mild jaundice, some providers will recommend placing your baby in indirect sunlight.
- In the case of severe jaundice, an exchange blood transfusion may be needed.
Complications
Luckily, with prompt treatment, jaundice is almost always treated successfully. When left untreated it can cause:
- Cerebral Palsy
- Deafness
- Kernicterus – when bilirubin reaches the brain, causing damage
Takeaways
- Jaundice is within the realm of normal for newborns but should be monitored closely.
- If jaundice is noticed in the first 24 hours of life, worsens rapidly, fails to respond to phototherapy, or lasts more than three weeks, additional testing may be suggested.
- If supplementation becomes necessary, do so after breastfeeding, to hasten the arrival of your milk, and to protect your milk supply.
- As always, listen to your gut and call your healthcare provider if you have additional worries.
Further reading:
- The Mayo Clinic
- American Academy of Pediatrics Clinical Practice Guide – Hyperbilirubinemia
- KellyMom – Breastfeeding a Baby With Jaundice (Resources)




Leave a Comment